Pioneering A New 3-D Cancer Model To Speed New Treatments
News Release
May 7, 2018
University of Virginia School of Medicine
Edited For Style and Length
A scientist at the University of Virginia School of Medicine, working with local biotech company HemoShear Therapeutics, has created a physical, three-dimensional model of a cancer tumor that can replicate the complex nature and behavior of a real tumor. The model will help researchers better understand the disease and accelerate the development of new and better treatments.
“This model enables us to understand the inner workings of tumors to systematically identify and test new ways to treat cancer,” said researcher Dan Gioeli of UVA’s Department of Microbiology, Immunology and Cancer Biology and the UVA Cancer Center.
Better Understanding Cancer
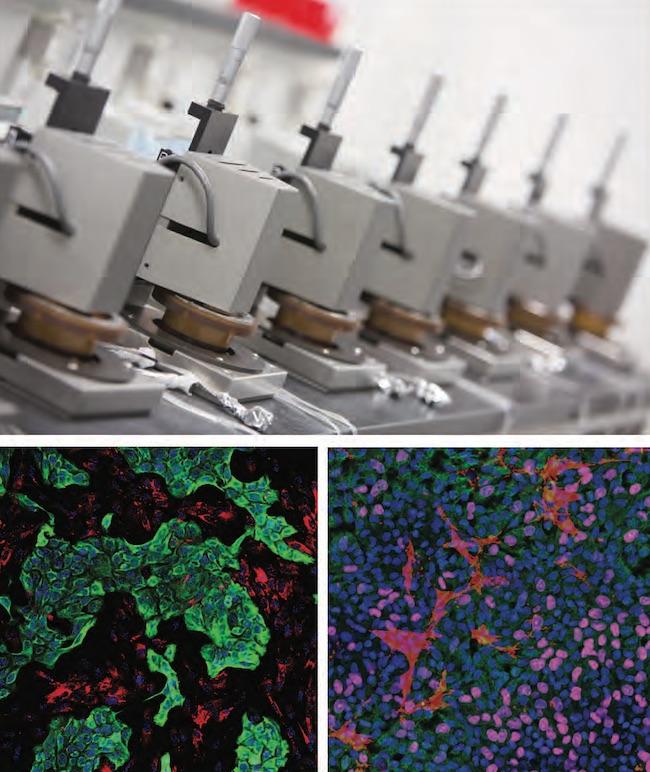
Top image: HemoShear Therapeutics Flow Devices used to recreate the tumor microenvironment using REVEAL-Tx with potential applications for creating patient avatars. Bottom left (pancreatic) and bottom right (lung) images: tumor and stromal cells are imaged following co-culture with blood vessel cells exposed to tumor hemodynamics.
Credit: Courtesy HemoShear Therapeutics
Gioeli’s model, made in collaboration with HemoShear, reflects the complexities of cancer by incorporating different cell types that are found in tumors. For example, it includes vascular endothelial cells, the cells that line blood vessels and are exposed to the tremendous shearing forces of blood flow.
Researchers will be able to manipulate the different components of the model in a way not possible with existing methods, according to HemoShear. This should provide important insights during the development of new treatments, Gioeli said.
“This model incorporates tumor hemodynamics and biological transport in a way that other tumor models do not,” he said. “We believe this model can be used for the rapid evaluation of novel precision therapies.”
Gioeli has worked as senior director of cancer biology at Charlottesville-based HemoShear while on sabbatical from UVA. He has a financial stake in the company.
HemoShear’s core technology was originally developed by two UVA researchers to create more accurate models of human disease for deeper understanding of how diseases develop and to discover safer and more effective drug therapies.
